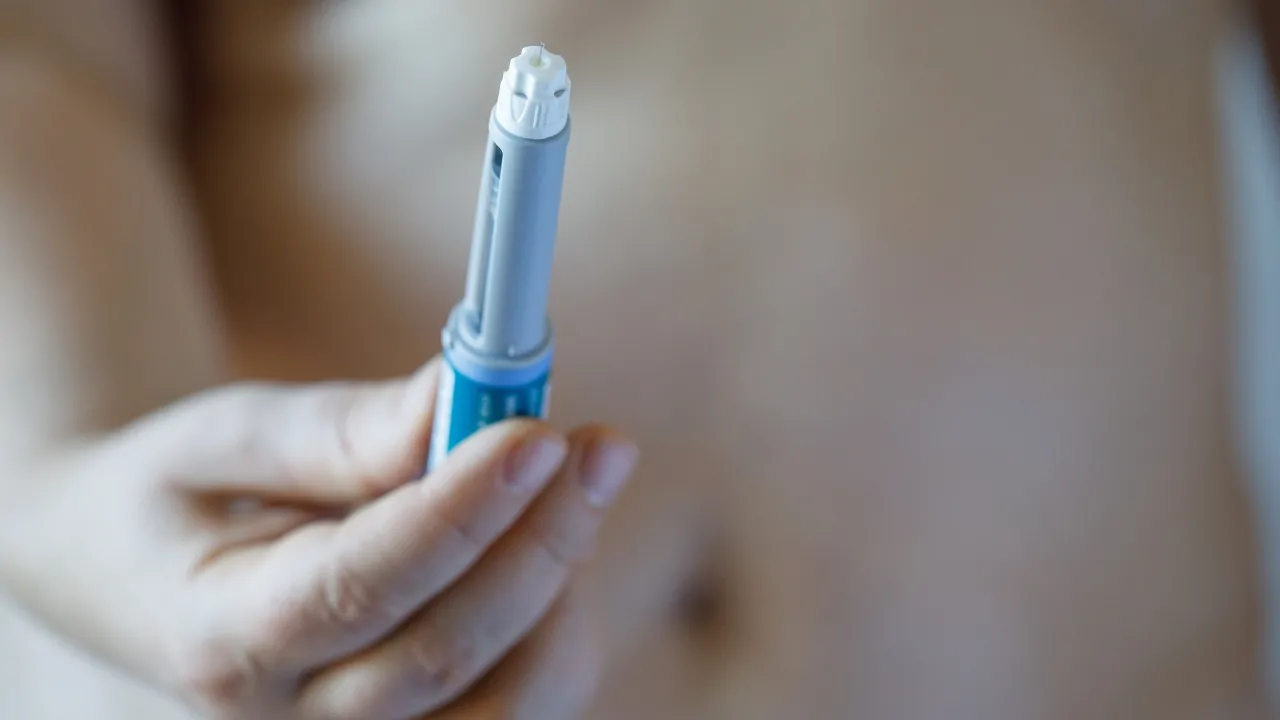
Semaglutide, a GLP-1 receptor agonist used in medications such as Ozempic and Wegovy, is widely known for treating diabetes and obesity.
New findings suggest that its effects may extend to mental health and addiction-related outcomes as well.
Recent observational research points to possible reductions in depression, anxiety, substance use problems, and self-harm risk among people taking the drug.
Support for that idea comes through two large studies, one focused on psychiatric outcomes and another centered on substance use disorders.
What the Major Mental-Health Study Found
A major study followed 95,490 Swedish adults diagnosed with depression or anxiety disorders between 2009 and 2022.
Researchers examined what happened during periods when the same individuals were taking semaglutide and compared those periods with times when they were not on the medication.
Results showed that semaglutide use was associated with a 42% lower risk of worsening mental illness.
Because the comparison was made within the same people across different treatment periods, the findings drew attention as a strong signal in favor of a possible psychiatric benefit.
Several of the most important outcome measures showed notable reductions:
GLP-1 drugs, as a broader group, were also associated with a lower risk of self-harm or suicidal behavior. That pattern matters because it suggests the observed benefit was not limited to only one symptom category.
Instead, results pointed to possible effects across multiple forms of mental-health deterioration, including mood symptoms, anxiety symptoms, addiction-related problems, and serious crisis outcomes.
Another reason these findings drew interest is that semaglutide is primarily known as a treatment for diabetes and obesity.
Psychiatric improvement was not the original purpose of the medication, yet the data suggested a meaningful association with better mental-health outcomes.
Such results raise the possibility that semaglutide may influence systems tied not only to metabolism, but also to mood regulation and behavioral control.
Why Researchers Think This Matters

Researchers believe these findings matter because semaglutide may influence brain pathways tied to reward, craving, mood, and stress response, not just appetite and metabolism.
Interest in that possibility has grown because addiction, depression, anxiety, and metabolic disease often overlap in the same patients.
A medication that acts across several of those pathways could eventually become valuable in a broader clinical context.
Several proposed brain-related effects help explain why scientists are paying close attention:
Addiction-focused reporting and earlier animal and human observational evidence have supported the idea that GLP-1 drugs may affect behaviors linked to compulsive use and emotional distress.
If semaglutide helps reduce craving or modifies how the brain responds to reward cues, that could help explain why lower risks were seen in substance use outcomes.
If it also influences stress and mood systems, that could help explain the reductions linked to depression and anxiety outcomes.
Patients with obesity or diabetes often struggle with overlapping mental-health challenges. Depression can worsen self-care.
Anxiety can complicate treatment adherence. Addiction can intensify medical risk and raise the chance of hospitalization, overdose, and suicide-related crises.
In that context, one medication potentially helping multiple connected conditions has become an important clinical question.
People looking into medical weight-loss treatment options can also find practical prescription information at medvidi.com.
Semaglutide Appeared Stronger Than Some Related Drugs
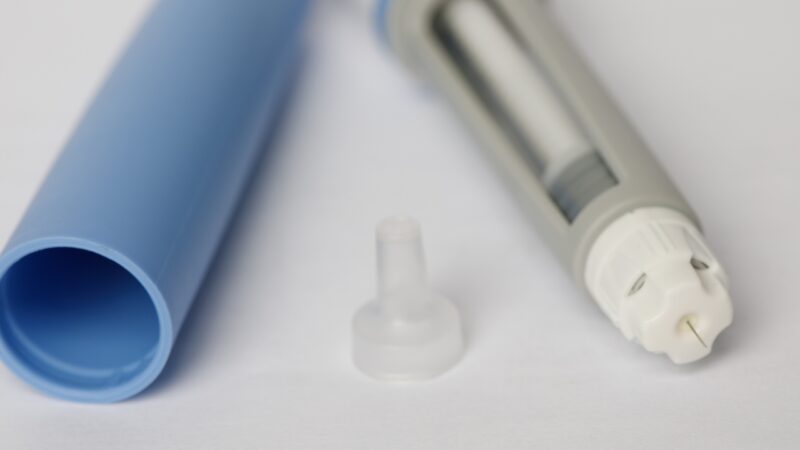
Results in the same reports suggested that semaglutide may have had a stronger association with mental-health improvement than certain related medications in the GLP-1 class.
Liraglutide was also associated with benefit, though the effect appeared smaller, at about an 18% lower risk of worsening mental illness.
By contrast, other GLP-1 drugs such as exenatide and dulaglutide did not show similarly strong reductions in mental-illness risk in the summarized reporting.
Differences among the drugs became more noticeable in the comparative pattern:
Such variation suggests outcomes may not be consistent across every drug in the GLP-1 category.
Medications in the same class can share broad mechanisms while still producing different clinical patterns.
In practical terms, that means semaglutide may be showing a stronger signal for mental-health and addiction-related benefits than some alternatives that act on similar pathways.
Caution is still needed when interpreting those comparisons. Observational data can point to meaningful differences, but it cannot fully explain why one drug appears stronger than another.
Dosing, patient selection, duration of treatment, and other clinical variables may all influence the pattern seen in the data.
Addiction Findings Add Another Layer
Starting a GLP-1 drug was linked with a 14% overall reduced risk of new substance use disorders and a lower risk of harm for those with existing use disorders. @SArunogiri @MonashUni https://t.co/WSAtewovnJ
— The Conversation – Australia + New Zealand (@ConversationEDU) March 5, 2026
Another major study added more evidence by examining substance use outcomes. Reporting on that research stated that starting a GLP-1 drug was linked to a 14% lower overall risk of developing a new substance use disorder.
Findings also suggested that GLP-1 treatment may help people who already have a substance use disorder by lowering the risk of severe complications and crisis events.
Among people already living with a substance use disorder, several outcome measures moved in a favorable direction:
The study data covered more than 600,000 U.S. veterans with diabetes. Investigators compared people who started GLP-1 drugs with people who started SGLT2 inhibitors.
That comparison is important because it placed GLP-1 treatment against another active diabetes medication group rather than against no treatment at all.
Results, therefore, suggested more than a broad health difference between treated and untreated populations.
A more detailed look at the numbers makes the clinical importance easier to see. Lower rates of emergency visits and hospital admissions suggest fewer destabilizing episodes tied to substance use.
Lower overdose rates and fewer suicidal thoughts or attempts point to a possible reduction in the most dangerous outcomes associated with addiction. A 50% reduction in deaths is especially striking, even though the result still needs confirmation in stronger trial settings.
Important Caveats
Important limits need careful attention. Neither study proves causation because both were observational.
Associations in large datasets can be valuable, but they do not establish direct cause and effect.
Researchers can measure patterns and compare groups, yet unmeasured differences may still influence the outcome.
Authors of the psychiatric study stated clearly that more randomized clinical trials are needed before stronger conclusions can be made.
Several cautions shape how these findings should be read:
Generalizability is another issue. Addiction-related findings may not apply equally to all populations because the cohort was made up mostly of older men with diabetes treated in the Veterans Affairs system.
Women, younger adults, people without diabetes, and patients outside that health system may not experience the same outcomes.
For that reason, broader studies will be necessary before the results can be applied confidently across the general population.
Mixed earlier research also matters.
Some prior work on GLP-1 drugs and mental health did not show such strong signals, which means current findings should be treated as promising rather than conclusive.
Strong observational results can open the door to new clinical questions, but trial data will need to confirm if semaglutide truly has a direct therapeutic effect on depression, anxiety, addiction-related harm, or suicidality.
FAQs
Summary
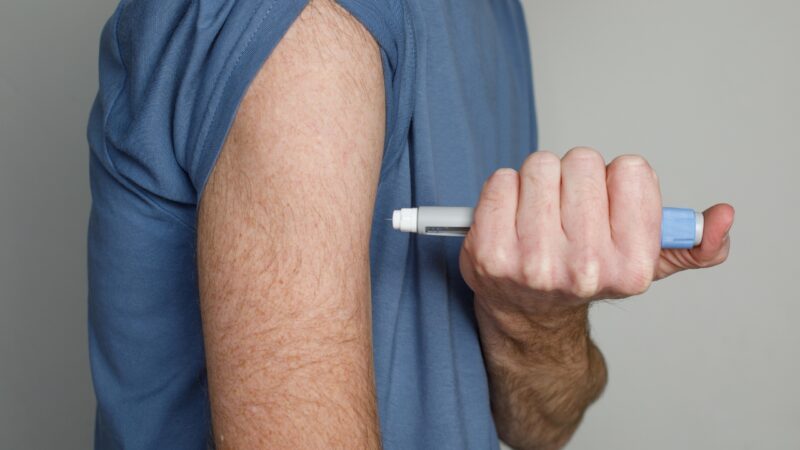
Growing evidence suggests that semaglutide may do more than help people lose weight or manage diabetes.
Large observational studies now indicate that it may also reduce the risk of depression, anxiety, self-harm, and addiction-related harms, with semaglutide showing especially strong signals in several measures.
Next steps call for rigorous clinical trials to determine if those benefits can be confirmed before semaglutide is treated as a psychiatric or addiction therapy on its own.