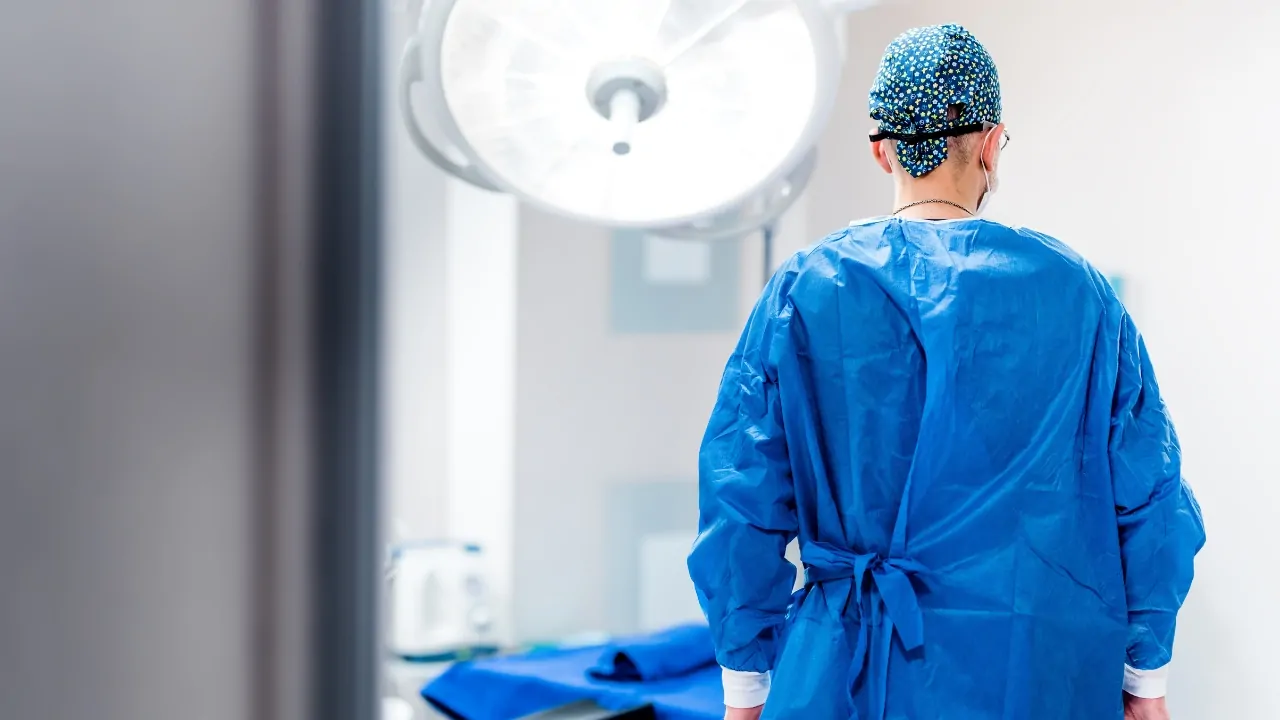
A patient waiting months for a hip replacement, knee replacement, cataract operation, cancer procedure, MRI, or CT scan is not facing a minor scheduling delay.
Canada’s wait-time problem is often described as a pandemic backlog issue, but that explanation is no longer enough.
Surgical volumes have increased, hospitals have reduced much of the COVID-19 backlog, and provinces have added capacity in several areas. Yet many patients still wait longer than they did in 2019.
A central question now faces Canada’s health-care system: Can community surgical centers cut wait times, or do they simply shift pressure inside a system already short on staff, space, and coordination?
Canada has become a major test case as provinces move selected procedures from hospitals to community-based surgical and diagnostic facilities.
Table of Contents
ToggleWhy Canadians Wait so Long for Non-Urgent Surgeries
“Non-urgent” surgery does not mean optional surgery. A hip replacement, knee replacement, cataract operation, or diagnostic scan may not require emergency care, but delay can still cause serious harm.
Months of waiting can mean pain, disability, lost income, dependence on family members, and worse health before treatment.
For patients in need of procedures like knee replacement surgery, these delays can directly affect mobility, independence, and quality of life.
Several pressures have pushed wait times upward. Underinvestment in facilities and technology limits capacity.
Workforce shortages leave hospitals and clinics without enough nurses, anesthesiologists, surgeons, imaging staff, and support workers.
Inefficient resource use creates bottlenecks. Rising demand adds more pressure. Pandemic backlogs intensified problems already present.
Recent elective-surgery data show how sharply access weakened after COVID-19:
International comparisons add another warning sign. In a 10-country comparison, Canada had the largest share of people waiting more than a year for elective surgery, at 20%. The United Kingdom followed at 19%, and Australia followed at 12%. Numbers like these point to a structural capacity problem, not just a temporary backlog. Recent national data shows a clear paradox. Canada has increased surgical volume since the height of the pandemic, but many patients still wait longer than they did in 2019. Hip and knee replacements show the problem most clearly: Cataract surgery came closer to recovery. In 2024, 69% of cataract surgeries were completed within the 16-week benchmark, compared with 70% in 2019. That suggests some areas can recover when procedure volume, staffing, and scheduling capacity line up. Other areas show continued strain: Diagnostic delays matter because imaging often determines diagnosis, treatment planning, and surgery scheduling. Longer waits for MRI and CT scans can slow care before a patient even reaches the surgical queue. Persistent waits are tied to more than COVID-19. Canada’s population is growing and aging. Patients often have more complex medical needs. Staffing shortages continue to limit capacity. Higher procedure volume alone has not solved the wait-time problem. For that reason, provinces are testing alternative surgical and diagnostic settings outside hospitals. Community surgical centers are non-hospital facilities that perform selected publicly funded procedures. Usually, they focus on routine or lower-complexity surgeries and diagnostic services such as: Policy logic is simple. Hospitals manage emergencies, intensive care, complex cases, inpatient beds, and unexpected disruptions. Community surgical centers can move selected planned procedures into settings less likely to be interrupted by emergency pressures. That can give hospitals more operating-room time for urgent and complex cases. A facility built around predictable procedures can organize staff, rooms, equipment, and scheduling around a narrower set of tasks. That can reduce cancellations, improve patient flow, and increase total procedure capacity. Staffing is the major risk. Clinics and hospitals often need the same nurses, anesthesiologists, surgeons, technicians, and recovery staff. Extra facilities may not add true capacity if they simply move workers out of hospitals. For community centers to help, hospitals and clinics need coordinated staffing rather than competition. Across Canada, alternative care settings are one part of a wider wait-time response. Better waitlist management, added imaging capacity, staffing plans, central intake systems, and quality oversight all matter as well. Ontario offers one of the clearest examples of a province betting on community surgical and diagnostic centers. A $125 million, two-year investment will add four new community surgical and diagnostic centers licensed to provide orthopedic surgeries. That plan is expected to support up to 20,000 additional publicly funded orthopedic procedures. Planned centers will perform hip and knee replacements, with new licences expected to begin in early 2026. Ontario’s stated goal is to raise the share of patients receiving orthopedic care within clinically recommended timeframes, moving it upward in the range of about 80% to 90%. Four sites are part of the plan: Ontario argues that community surgical and diagnostic centers are already a major part of provincial care. Such centers have operated there for more than 30 years. More than 900 community surgical and diagnostic centers operate in Ontario, most focused on diagnostic imaging. Provincial wait-time data gives Ontario its strongest argument: Ontario’s safeguards are meant to protect public access. New facilities must provide staffing plans designed to protect public hospital staffing. Centers must report into the provincial wait-times information system. Centers must take part in regional central intake systems where available. Quality oversight is required through Accreditation Canada’s quality-assurance program. Ontario also says patients cannot pay to receive insured services faster than others. Centers also cannot refuse insured services to patients who decline uninsured upgrades. Rules like these are meant to protect equal access while allowing more procedures outside hospitals. Saskatchewan offers a more cautious example. Its plan includes expanding private clinics that perform publicly funded procedures as part of a broader health-care strategy. Provincial targets for 2028 are ambitious: Saskatchewan already uses private providers for surgeries involving joints, eyes, and the vascular system. Plans call for greater use of private clinics to meet surgical targets. Controversy around Saskatchewan’s plan centers on staffing, capacity, and public confidence. Experts have questioned the likelihood that reliance on private clinics will meet provincial targets. Concerns also focus on how private delivery could affect public hospitals. Public funding may stay in place, but care shifts into clinics outside hospital walls. That shift can expand capacity if it adds operating time, better scheduling, and more procedure slots. Risk increases if it pulls scarce workers out of hospitals already struggling to staff operating rooms, emergency departments, and inpatient units. Workforce shortages are the key issue. If staffing is the true bottleneck, more clinic space will not automatically shorten waits. A new operating room cannot perform surgery without nurses, anesthesiologists, surgeons, technicians, cleaners, and recovery staff. Saskatchewan’s plan may be judged by system-wide results, not design promises. Patients will want to know if waits shrink across the system, not only for selected procedures in selected clinics. Community surgical centers are most persuasive when they focus on high-volume, predictable procedures. Hip replacements, knee replacements, cataract surgery, endoscopies, MRI scans, and CT scans fit work that can often be scheduled more efficiently outside a hospital. Specialized centers can organize around repetition and predictability. Teams may complete procedures with more consistent scheduling. Operating-room turnover time may improve. Hospital-based cancellations may fall. Routine care can be separated more clearly from emergency pressures. Ontario’s model gives the strongest pro-expansion case because it links community centers to measurable added volume: National data support the case for added capacity. Even after higher surgical volumes in 2024, benchmark performance for hip and knee replacements stayed below 2019 levels. Canada is doing more procedures, but demand and system pressure are still outpacing recovery in major categories. Community-based surgical clinics can increase capacity for less complex surgeries, but coordination is essential. Hospitals and clinics need shared planning, so staff are not simply pulled out of one setting and placed into another. Central intake, wait-time reporting, quality oversight, and staffing protections can determine how useful these centers become. The best-case scenario is not a two-tier workaround. The best-case scenario is an integrated public system that uses community centers for appropriate procedures, while hospitals focus on emergencies, complex care, and patients needing inpatient support. Surgery, diagnostic wait times continue to grow across Canada: report https://t.co/tzZano9Fml — CTV News (@CTVNews) September 26, 2025 Community surgical centers could help Canada reduce waits for specific procedures, especially standardized, lower-risk surgeries and diagnostic services. They can add predictable operating capacity, reduce some hospital cancellations, and move routine care into settings designed for efficient scheduling. Evidence also shows that Canada’s problem is larger than a shortage of operating rooms. Workforce shortages, aging patients, greater medical complexity, inefficient waitlist management, and uneven regional capacity all contribute to long waits.
Canada Is Doing More Procedures, but Wait Times Are Still Worse than Before the Pandemic
What Are Community Surgical Centers?
Ontario is The Pro-Expansion Case
Saskatchewan as The Cautionary Case
Strongest Argument for Community Surgical Centers
FAQs
Closing Thoughts
Related Posts: