Cancer care traditionally begins after symptoms appear and a tumor is already present. A growing area of research is trying to change that timeline completely. Scientists are exploring ways to detect and manage cancer risk decades before the disease actually forms.
This concept, often called cancer interception, focuses on identifying the earliest biological changes that eventually lead to cancer and addressing them early enough to prevent full disease development.
The idea is straightforward but ambitious: instead of treating cancer once it exists, reduce the chance it ever appears. Advances in genetics, molecular biology, and diagnostic testing are making this approach increasingly realistic.
Table of Contents
ToggleEarly Biological Clues Researchers Are Tracking
Cancer rarely develops overnight. Cells gradually accumulate mutations, and some of those mutations give certain cells a survival advantage. Over time, these altered cells can multiply and eventually form tumors.
Researchers are paying close attention to several early indicators:
Early Indicator
What It Means
Genetic mutations in cells
Small DNA changes that accumulate with age
Precancerous lesions
Polyps, abnormal moles, or tissue changes
Clonal cell populations
Groups of mutated cells are expanding silently
Chronic inflammation
Conditions that can accelerate mutation growth
These warning signs can exist for years or even decades before cancer becomes clinically detectable.
Large genetic studies show that as people age, many develop small populations of mutated cells, particularly in the blood. These are called clones. Some clones remain harmless, while others increase cancer risk depending on genetics, environmental exposure, and immune system response.
Long-Term Studies Are Revealing Risk Patterns

One notable long-term study followed about 7,000 women over 16 years. Researchers tracked how mutations behaved over time and how environmental factors influenced them.
Key observations included:
Because these changes can now be measured through blood tests, doctors may eventually monitor cancer risk similarly to how they track cholesterol or blood pressure.
Cancer Develops Gradually, Not Suddenly
This research reinforces a major shift in understanding cancer. It is usually not a sudden event. Instead, it is a multi-stage biological process with detectable early signals.
That realization has opened the door to new diagnostic technologies, particularly blood-based screening tests designed to catch cancer extremely early.
Blood Tests That May Detect Cancer Years Earlier
One of the most promising developments is multi-cancer early detection (MCED) testing. These tests search for circulating tumor DNA (ctDNA) in the bloodstream.
Even very small or early-stage cancers release tiny DNA fragments into the blood. Detecting these fragments could allow intervention long before symptoms or imaging changes appear.
Here is why early detection matters:
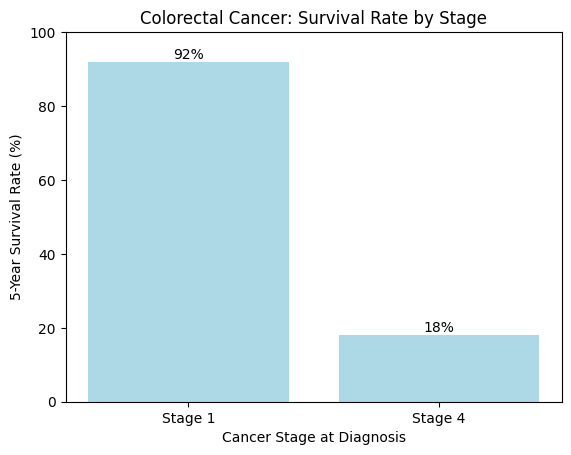
This dramatic difference shows why earlier detection can significantly improve outcomes.
However, MCED testing is still evolving. Some cancers are missed, and positive results often require further imaging or biopsies for confirmation.
Learning From Heart Disease Prevention
Cardiology already uses prevention-based models successfully. Doctors estimate heart attack risk using factors like:
Preventive medications such as statins are often prescribed years before any symptoms occur.
Cancer researchers hope to develop a similar predictive framework by combining:
Risk Factor Category
Examples
Genetic markers
DNA mutations, inherited risk
Environmental exposure
Smoking, pollution, diet
Biological signals
Inflammation markers, ctDNA
This could allow tailored prevention strategies rather than reactive treatment.
Important Differences Between Cancer And Heart Disease
Despite similarities in prevention strategy, cancer behaves less predictably than cardiovascular disease.
Some early lesions never progress. Others grow slowly or even regress. That unpredictability makes intervention decisions more complex.
Another concern is overdiagnosis. Being told you are at an elevated cancer risk while feeling completely healthy can create psychological stress without guaranteed benefit.
Ethical And Practical Challenges
Preventive cancer medicine raises several difficult questions.
False-positive test results can lead to:
Access is another concern. If advanced screening remains expensive or privately funded, it could widen health inequalities, especially in lower-income populations.
Regulatory agencies are currently studying how these tests should be used safely. Reliability standards, follow-up protocols, and cost considerations are all under evaluation.
National Health Systems Are Preparing For Earlier Detection
It’s World Cancer Day and our National Cancer Plan:
💰Invests £2.3 billion in 9.5 million more tests & scans
🧑⚕️Sends cancer specialists to rural & coastal areas
🤖Delivers 500,000 robotic surgeries
👫Helps 3 in 4 patients survive 5 years after diagnosishttps://t.co/OtI5013vkg— Wes Streeting (@wesstreeting) February 4, 2026
Some countries are already planning expanded diagnostic programs. For example:
These efforts suggest early cancer interception could become part of routine healthcare in the future.
What This Means Moving Forward
Cancer prevention research is shifting from late-stage treatment toward early biological monitoring. Evidence increasingly shows cancer develops gradually, often over decades.
Detecting and managing risk earlier hasthe potential to reduce mortality significantly.
However, scientific, ethical, and economic challenges remain. The balance between early detection benefits and the risks of unnecessary intervention still needs careful evaluation.
The overall direction is clear: future cancer care may focus less on reacting to tumors and more on preventing them from forming at all.








