Denture materials are changing fast because the old problem has never been small: a denture has to sit on living tissue, handle chewing forces every day, resist staining, avoid roughness, and still feel natural enough for someone to eat and speak with confidence.
New 3D printed denture materials are attracting attention because they may improve fit, comfort, repairability, and durability, while also making replacement dentures easier to reproduce from a saved digital file.
The promise is real, but so are the limits. Better resins, nanofillers, printing settings, and post-curing methods all matter.
Table of Contents
ToggleWhat Makes 3D Printed Dentures Different?
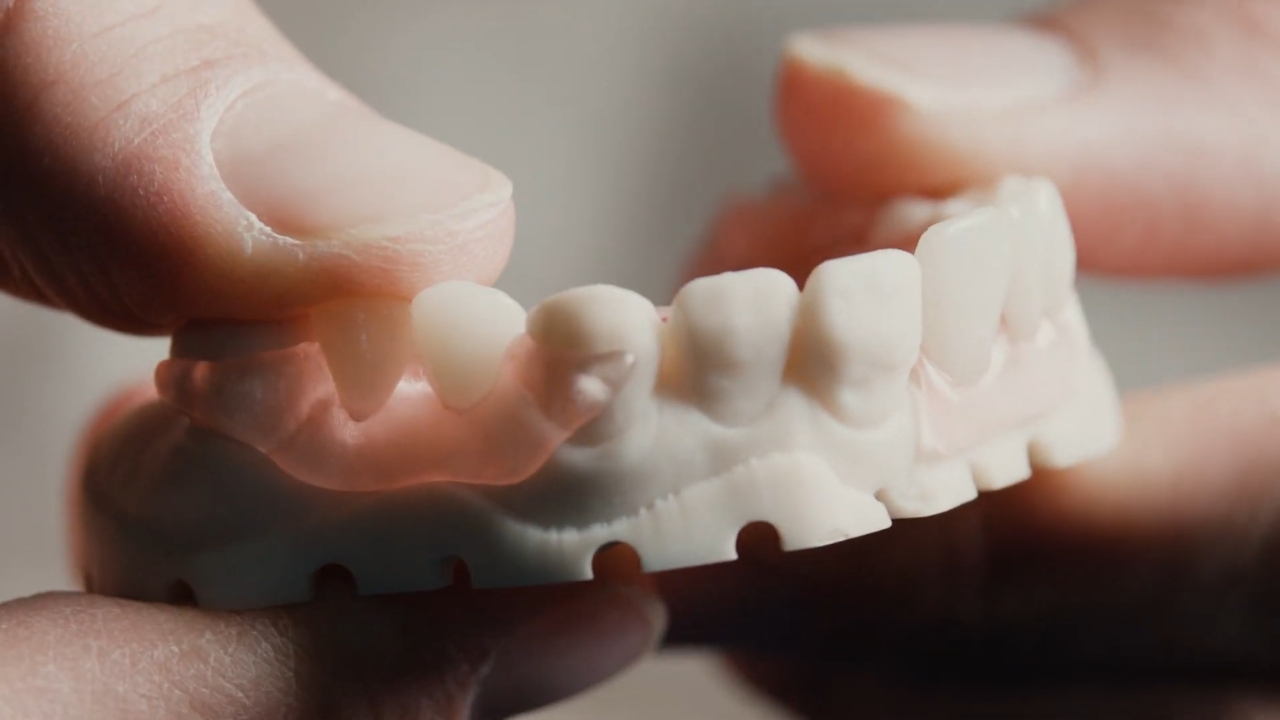
Traditional dentures are usually made through hand-based laboratory steps using wax try-ins, stone models, acrylic processing, trimming, and polishing. Skilled technicians can produce excellent results, but the process depends heavily on manual workflow.
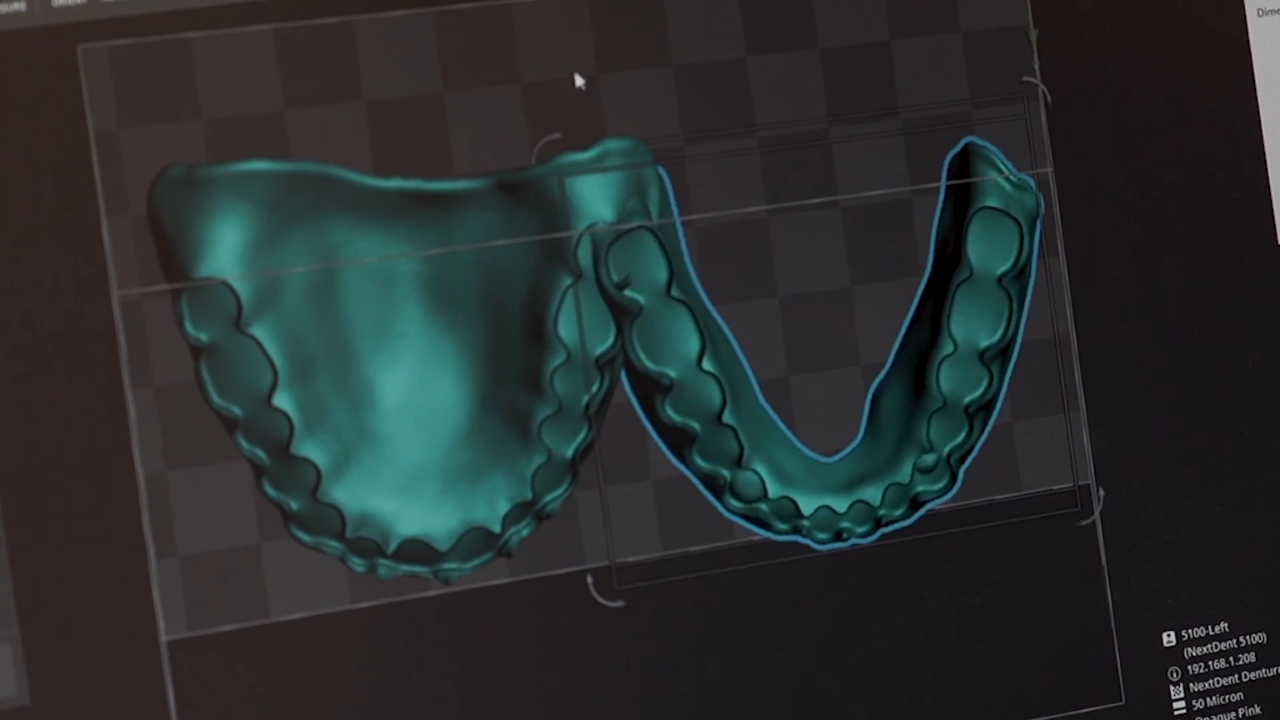
3D printed dentures start with digital information. A clinician scans the mouth or captures impressions, designs the prosthesis with software, then prints the denture base and teeth from approved dental resins.
FDA classification records for additively manufactured resin denture teeth describe a digital patient scan paired with software and a 3D printer that builds patient-matched denture teeth layer by layer.
That digital file can be stored. If a denture breaks or gets lost, a lab may be able to reproduce it without restarting every clinical step from zero.
Clinics that already work with digital planning and restorative dentistry, such as lemaclinic.com, show why patient records, scans, and treatment design are becoming more central to modern dental care.
Conventional Dentures Vs. 3D Printed Dentures
Feature
Conventional Dentures
3D Printed Dentures
Main workflow
Manual lab processing
Digital design and additive manufacturing
Fit control
Depends on impressions, lab technique, and adjustments
Depends on scan accuracy, software design, printer calibration, and curing
Replacement
Often requires new impressions and lab work
A digital file may allow faster reproduction
Material concerns
Acrylic shrinkage, staining, roughness, and fracture risk
Layer bonding, resin strength, surface finishing, and long-term aging
Clinical promise
Familiar, widely used, proven over time
Faster workflow, repeatability, and possible material customization
How New Materials Aim To Improve Comfort
Comfort begins with fit. A denture base must adapt closely to the ridge and soft tissue without creating pressure spots. Digital denture workflows can help because design software allows precise border shaping, thickness control, and repeatable fabrication.
A 2026 narrative review in The Saudi Dental Journal found that digitally fabricated complete dentures can show comparable or better outcomes in retention, adaptation, and patient satisfaction, while reducing clinical visits and post-insertion adjustments.
The same review also warned that cost-effectiveness, material behavior, and long-term performance still require stronger evidence.
Comfort also depends on surface quality. A polished denture base feels smoother against the tongue and cheeks. Smoother surfaces can also make hygiene easier.
Rougher denture surfaces tend to trap microorganisms and stains, which can lead to odor, inflammation, and sore tissue.
Durability Is Where The Science Gets More Complicated
Early 3D printed denture resins were often criticized for lower mechanical performance compared with heat-cured or milled materials. Recent materials are improving, but the field remains uneven.
A 2025 Scientific Reports study compared 3D printed and conventional denture base materials for durability, water absorption, and solubility.
The authors noted that previous research has reported mixed findings, with many studies finding lower physicochemical properties for printed denture base materials compared with traditional methods.
That does not mean printed dentures are weak by default. It means the final result depends on resin chemistry, printer type, build orientation, layer thickness, post-curing, polishing, and cleaning habits.
The Role Of Nanofillers In Stronger Denture Resins
One of the most active research areas involves adding tiny reinforcing particles to printable resin. Researchers are testing zirconia, titanium dioxide, silicon dioxide, zinc oxide, silver-based particles, nanodiamonds, glass fillers, and other additives.
A 2024 review in Science Progress reported that PMMA remains a long-standing denture base material, but its limits have pushed research toward improved 3D printed resins.
The review found that nanoparticles can improve performance compared with unmodified resins, especially when surface treatments help particles bond better with the polymer matrix.
Why Nanofillers Matter
Results vary by filler type and concentration. More filler does not always mean better performance. Too much can clump, weaken the resin, affect appearance, or raise biocompatibility concerns. A denture base gets much of the attention, but denture teeth also wear, chip, and fracture. Printed teeth must survive chewing forces and sliding contact with opposing teeth. A 2024 study in Polymers compared 3D printed resin denture teeth with prefabricated denture teeth. The authors found that printed resin teeth showed adequate fracture resistance for clinical use, although further material refinement could improve performance against certain conventional options. That finding is important because dentures are a system. A strong base, paired with teeth that wear too quickly, can still create problems. Bite height can change. Chewing efficiency can drop. Sore spots can appear because forces shift. Denture stomatitis, a common inflammation under dentures, is often linked with microbial buildup, especially Candida albicans. Material surface roughness, poor cleaning, overnight wear, dry mouth, and age-related health changes can all raise risk. A 2024 MDPI study on nanoparticle-modified 3D printed denture base resins found that denture cleansers can affect color and surface roughness across both modified and unmodified materials. The study also noted that rougher surfaces can encourage microbial plaque accumulation and make plaque harder to remove. Antimicrobial additives may help, but they require caution. The 2024 Science Progress review emphasized that nanoscale fillers need long-term biocompatibility testing, mechanical aging studies, and toxicity evaluation before broad clinical use. Patients are unlikely to ask about zirconia nanoparticles or polymer networks. They care about the daily experience. A major caveat remains: the dentist and laboratory still matter. Poor scanning, rushed design, inadequate curing, or weak finishing can erase material advantages. 3D printed denture success depends on process control. A lab cannot treat every resin the same way. Each material has a validated workflow, including print orientation, washing time, post-curing time, light intensity, and finishing protocol. FDA classification also matters because intraoral dental materials must meet medical-device requirements. A resin meant for models or surgical guides is not automatically suitable for long-term denture wear. The denture market is moving toward hybrid workflows. Some cases may use milled bases with printed teeth. Others may use printed bases reinforced with nanofillers. Some labs may combine digital try-ins, printed prototypes, and final dentures made from higher-strength materials. The most useful future materials will probably share 4 traits: The field is not only chasing stronger dentures. It is chasing better predictability. New 3D printed denture materials could improve comfort and durability, especially as resin chemistry, nanofillers, and digital workflows mature. The strongest promise lies in better fit, easier replacement, cleaner production, and materials engineered for specific clinical needs. Still, printed dentures are not automatically superior. Long-term clinical evidence, careful material selection, proper curing, and skilled dental design remain essential. For patients, the best result will come from combining newer materials with experienced prosthodontic care.
Denture Teeth Need Strength Too

Hygiene, Biofilm, And Antimicrobial Materials
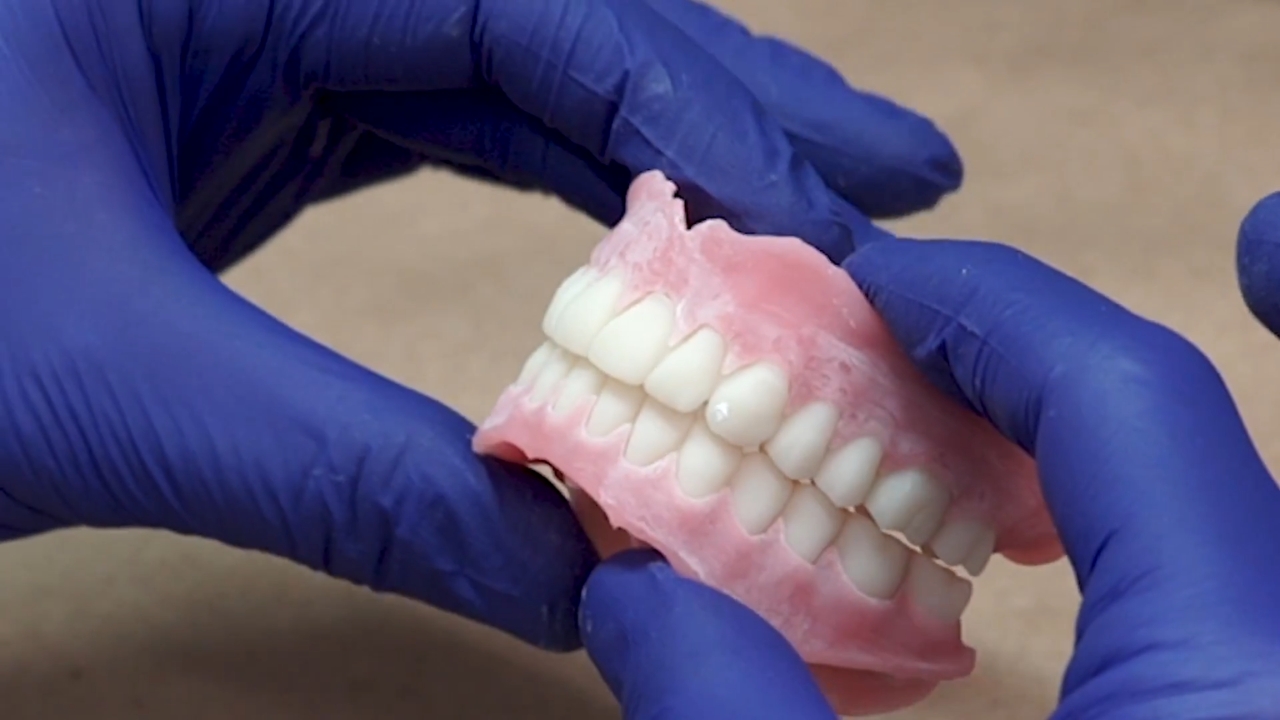
What Patients Could Notice First
What Dentists And Labs Still Need To Watch
Why The Next Few Years Could Be Important
Summary
Related Posts:








