Indirect contact from dynamic knee valgus (a knock‑knee posture), shallow knee flexion, and improper trunk posture are responsible for about 88 % of sports‑related ACL injuries, according to NCBI.
Secondary risks include weak muscles, poor neuromuscular control, and an increased Q‑angle; women’s risk is up to eight times higher than men’s.
The injury rate has risen roughly 1.3 % per year among collegiate athletes in the United States, and professional athletes experience incidences ranging from 0.15 % to 3.7 %.
Returning to pre‑injury performance isn’t guaranteed; only about 65 % of athletes regain their previous level, and reinjury rates can reach 15–21.9 %. Surgery remains the gold‑standard treatment, but rehabilitation is where long‑term functional recovery happens.
Traditional physiotherapy focuses on strengthening, range of motion (ROM), and proprioception, yet monotony and pain often dampen patients’ motivation.
Table of Contents
ToggleWhy Traditional Rehab Needs an Upgrade
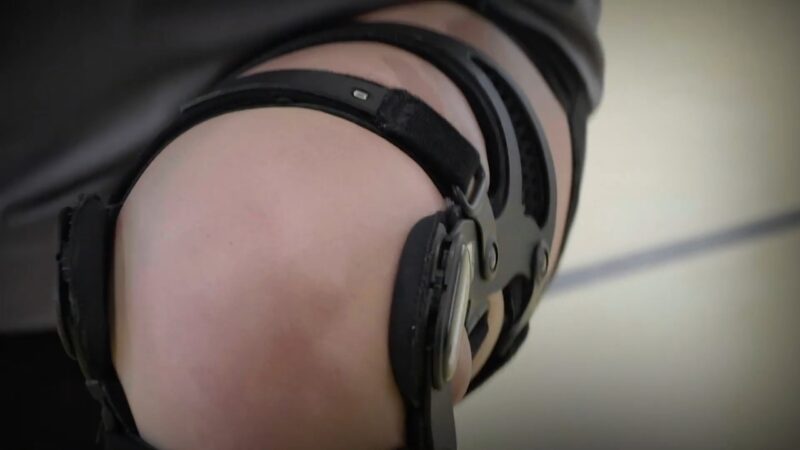
Conventional ACL rehabilitation involves weeks of repetitive exercises that strengthen the quadriceps and hamstrings, restore knee ROM, and train balance. These programs work, but they can be tedious.
Psychological factors such as fear of re‑injury, boredom, and the sense that progress is slow undermine adherence. When adherence suffers, so do outcomes; research shows that only 43 % of patients stick with traditional home‑exercise routines.
Meanwhile, clinicians continue to explore ways to make rehab engaging without sacrificing therapeutic rigor. Virtual reality (VR) offers a promising solution.
How VR and Gamification Work
VR therapy uses interactive software to immerse patients in digital environments. Non‑immersive VR (NIVR) displays 2‑D worlds on a screen and uses a controller or joystick. Immersive VR (IVR) uses head‑mounted displays with surround sound to let users see and hear 360‑degree environments.
Both types incorporate gamification, scoring points, unlocking achievements, and advancing through levels, to turn mundane exercises into fun tasks. When rehabilitation feels like a game, patients feel autonomous, competent, and connected.
One study found that gamified exercises increased adherence to home therapy programs to 87 %, compared with 43 % for traditional routines.
The technology is more than a flashy distraction. Brain‑imaging studies show that VR‑based rehabilitation increases activity in regions responsible for attention and focus. Patients become so engrossed in catching virtual objects or navigating digital obstacle courses that they feel less pain.
This pain modulation matters because it allows them to move through larger pain‑free ranges of motion and perform more repetitions, accelerating recovery.
What Research Says About VR for ACL Rehabilitation
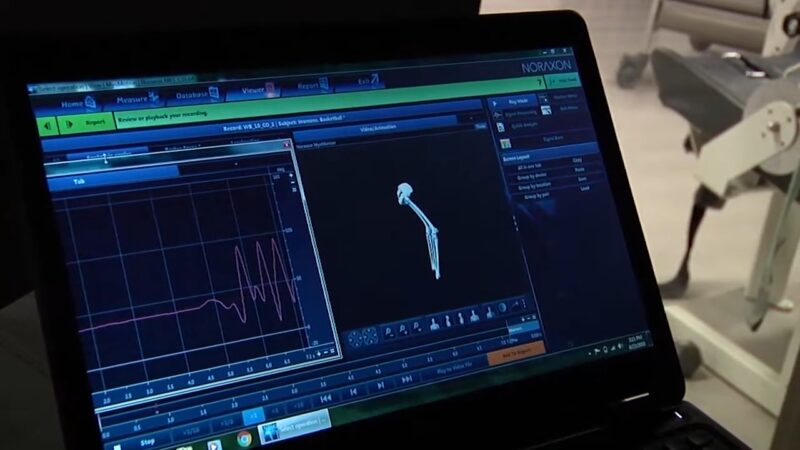
The most comprehensive evidence to date comes from a 2024 systematic review and meta‑analysis of nine randomized controlled trials involving 330 participants (average age ~27; 85 % men).
The researchers compared virtual reality–based therapy (VRBT) with classical physiotherapy for patients recovering from ACL injuries. They found that VRBT:
These improvements came with no reported adverse events, and the intervention appeared as a valuable complement to standard physiotherapy rather than a replacement. The meta‑analysis concluded that VRBT is an effective tool to include in ACL rehabilitation programs.
A separate study examining mixed‑reality exergames noted that standard rehabilitation often doesn’t fully prepare athletes for the complex demands of sport; only 65 % return to their previous performance level.
To address this gap, researchers developed a user‑centered exergame that blended strength, balance, endurance, and reaction training.
During development, focus groups revealed that both patients and physiotherapists wanted engaging, adjustable games that mimic sports tasks.
The final exergame allowed therapists to control difficulty levels and offered mini‑games for endurance and skills, showing potential for broader deployment.
Real‑World Adoption: Beyond the Lab
Evidence is one thing; implementation is another. Clinicians are beginning to integrate VR into their rehabilitation protocols. At the University of Florida, doctoral students use Meta Quest 3S headsets to simulate lifelike rehab scenarios.
The immersive technology allows students to gamify physical therapy, helping patients increase their range of motion and manage pain through environmental distraction. The program teaches future athletic trainers to guide patients through VR exercises tailored to individual needs.
For instance, a tennis player rehabbing in an urban setting can train virtually on a court that matches their sport.
Alex Alvarez, an athletic trainer in the U.S. Marine Corps and a graduate of the program, uses VR to replicate sport‑specific drills. He notes that patients can practice landing techniques or agility drills in a controlled virtual environment before returning to the field.
Clinicians also see psychological benefits: VR distracts patients who are fixated on pain, allowing them to move through larger pain‑free ranges of motion. Although cost and limited research still hinder widespread adoption, these educational initiatives suggest VR is poised to become a standard part of rehabilitation.
Other clinics report similar success. A major review of 72 clinical studies showed that VR significantly improves upper‑limb function and daily activities. Another analysis of 37 studies involving more than 1,000 patients found that VR‑based treatments improved motor function better than traditional therapy.
Gamified exercises are also associated with higher adherence rates and reduced pain. These results underpin the American Physical Therapy Association’s endorsement of VR in outpatient clinics.
How VR Helps You Heal
The magic of VR‑guided rehabilitation lies in four mechanisms:
- Immersive distraction: By transporting patients into engaging virtual environments, VR shifts attention away from pain. This distraction lowers perceived pain and encourages movement.
- Gamified motivation: Points, challenges, and level‑ups make repetitive exercises fun and satisfying. Gamification taps into the psychological need for autonomy, competence, and connection, resulting in higher adherence.
- Augmented feedback: VR provides real‑time visual and auditory feedback on movement accuracy. Seeing one’s movements mirrored in the virtual world helps patients correct form and develop proper movement patterns.
- Safe simulation: Virtual scenarios let patients practice sport‑specific tasks, such as cutting, jumping, or pivoting, without the risk of physical collisions. This controlled exposure reduces fear of re‑injury and improves dynamic balance and proprioception. Customizable difficulty levels allow therapists to progressively challenge patients while maintaining safety.
Looking Beyond Sports: Falls and Everyday Injuries

While athletes often grab headlines, ACL injuries and other knee traumas frequently occur during everyday activities such as slipping on ice, missing a step, or tripping over an obstacle.
These accidents can take people out of work for months, leading not only to medical costs but also to lost income.
If your knee injury resulted from a negligent property owner or unsafe conditions, you may be entitled to compensation that covers both medical expenses and the wages you missed during recovery. Knowing your rights and how to recover lost wages after a fall can ease the financial burden while you focus on healing.
Virtual reality isn’t limited to ACL rehabilitation either. Patients recovering from strokes, chronic back pain, and other musculoskeletal conditions use VR to manage pain and improve functional outcomes. For those who can’t attend clinics, at‑home VR platforms paired with tele‑rehabilitation could offer accessible therapy sessions.
Conclusion
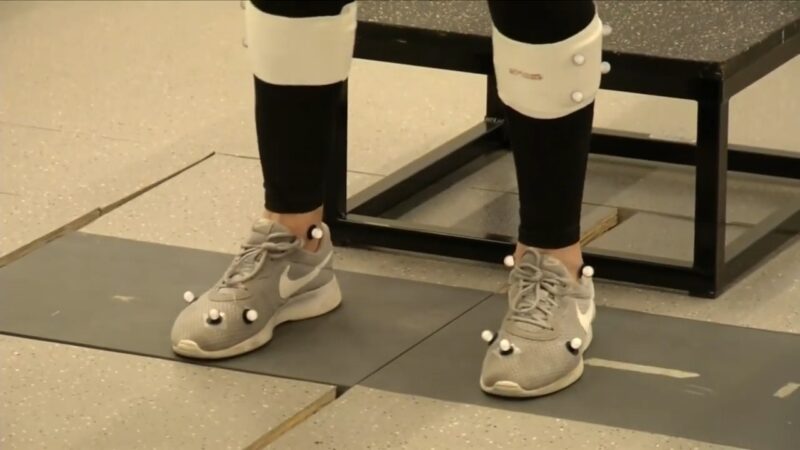
ACL injuries can derail an athlete’s season or disrupt an active lifestyle, and the long road back to health is often hampered by pain, boredom, and fear.
The latest research paints an encouraging picture: VR‑based rehabilitation significantly reduces pain, improves knee function, increases strength and ROM, and enhances dynamic balance.
Immersive games turn mundane exercises into engaging challenges, boosting motivation and adherence.
Real‑world programs like those at the University of Florida are preparing clinicians to harness this technology, while exergame developers design user‑centered workouts tailored to the demands of sport.